Translate this page into:
Male infertility – Laparoscopic approach in a case of persistent Müllerian duct syndrome

*Corresponding author: Pamoti Ravi Kumar, Department of Surgery, Ganni Subhalakshmi Medical College, Rajahmundry, Andhra Pradesh, India. drsamirnayak@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Kumar PR, Swathi T, Nayak SR. Male infertility – Laparoscopic approach in a case of persistent Müllerian duct syndrome. J Reprod Healthc Med. 2025;6:9. doi: 10.25259/JRHM_18_2023
Abstract
Persistent Müllerian duct syndrome (PMDS) is characterized by the persistence of Müllerian derivatives in a genotypically and phenotypically normal male. These patients have 46 XY karyotypes with normal male external genitalia, virilization, unilateral or bilateral undescended testes, bilateral fallopian tubes, a uterus, and an upper vagina draining into a prostatic utricle. We report a 25-year-old male on evaluation for primary infertility who was found to have bilateral cryptorchidism with a uterus and bilateral fallopian tubes. The laparoscopy helped us with the diagnosis, documentation of the findings, and to proceed for total hysterectomy and bilateral salpingectomy with left orchidopexy. PMDS should be considered for patients with bilateral cryptorchidism in adults. The radiological evaluation and diagnostic laparoscope are recommended for the diagnosis and subsequent counseling to the patient and family.
Keywords
46 XY phenotype
Müllerian inhibiting substance
Persistent Müllerian duct syndrome
INTRODUCTION
Persistent Müllerian duct syndrome (PMDS) is a form of male pseudohermaphroditism in normally virilised XY genotype individuals. They develop both Wolffian and Müllerian structures which is characterized by presence of uterus and fallopian tubes in genotypically normal male. First described by Nelson in 1939.[1] It is caused by either less amount of Müllerian inhibiting substance (MIS) or dysfunction of Müllerian inhibiting substance receptor on target organ. PMDS is often a late discovery during intraoperative or while investigating for undescended testes. Here we are presenting case of PMDS in a 25 year old male with bilateral undescended testis.
CASE REPORT
A male person with 46 XY chromosomes who has female reproductive organs is said to have PMDS, an uncommon developmental abnormality.
The primary cause of PMDS is a mistake in the anti-Müllerian hormone (AMH) type II receptor, and the true incidence is not known to be a deficiency in the generation of AMH from Sertoli cells.
A 25-year-old male presented to surgery clinics for evaluation of primary infertility. He noticed an absence of testis emptiness in the scrotal sac just 3 years prior. He had a history of surgery in the right inguinal region at the age of 3 years, for which details were not available.
On physical examination, the patient had normal secondary sexual characteristics with a male pattern of external genitalia well-developed beard, and moustache. The genital examination revealed the absence of both the testis even if the scrotal sac was well developed. There was an irreducible swelling of size 2 × 2 cm, which clinically appears as testis noted in the left inguinal region, firm in consistency. Penis appears normal as per age. The family history of the patient was nil significant.
On further evaluation with abdominal ultrasound (USG), bilateral testes were not visualized in the scrotum or the groin region. Bilateral spermatic cords could not be traced out. The tubular structure appears to be the uterus and the cervix was visualized just behind the urinary bladder [Figure 1]. The radiologist team suggested a magnetic resonance imaging (MRI) scan for further definition.
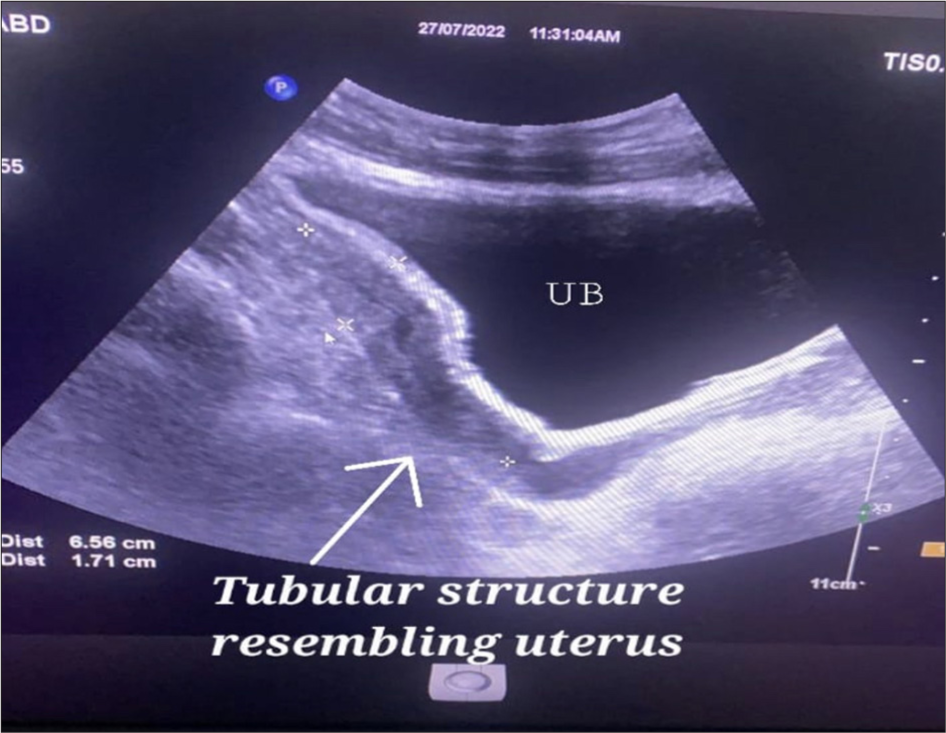
- Ultrasound image of patient showing tubular structure like uterus and cervix behind the urinary bladder.
MRI revealed a dilated tubular structure resembling a uterus noted posterior to the bladder measuring 4 × 2.4 cm; distally, this structure is medial to the vas deferens and is seen opening into prostatic utricle – likely paramesonephric duct remnant. Bilateral undescended testis, the right testis measures 3.2 × 1.4 cm located in the anterior right iliac fossa, and the left testis measures 3.6 × 1.4 cm in the left inguinal region. The final imaging impression was bilateral ectopic undescended testis with paramesonephric duct remnant [Figure 2].
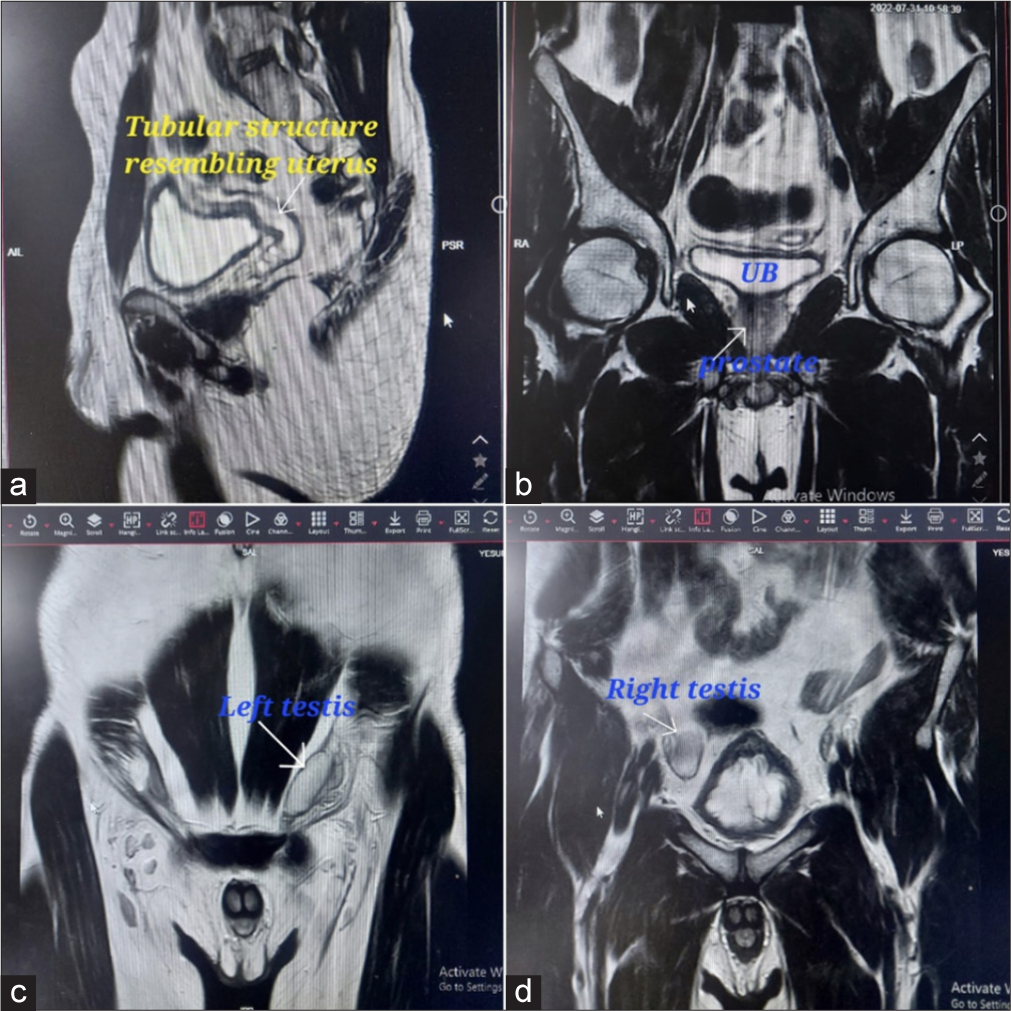
- Magnetic resonance image of patient showing (a) uterus behind urinary bladder (b) prostate (c) left testis in the left inguinal region (d) right testis in right iliac fossa anteriorly.
The patient was then subjected to further hormonal analysis and serum markers to know the cause of undescended testis and exclude malignancy. Serum markers reported as serum alfa fetoprotein: 4 ng/mL (0–40 ng/mL), serum beta human chorionic gonadotropin: 0.2 mIU/mL (<2 mIU/mL), and serum lactate dehydrogenase: 100 U/L (105–333 U/L) which ruled out testicular malignancy. The serum testosterone – 544 (300–1,000 ng/dL) and dihydrotestosterone (DHT) – 20 (14–77 ng/dL) suggested the male phenotype. The AMH was found to be <0.01 pmol/L. It is found to be too low, causing non-regression of the Müllerian duct to leading to the persistence of female reproductive organs in the patient.
The genetic karyotyping suggested 46 XY (normal male karyotyping), and the semen analysis showed azoospermia. After standard pre-operative preparation and pre-operative counseling, the patient was subjected to diagnostic laparoscopy. The laparoscopy finding was the right testis, which was intra-abdominal in the right iliac fossa, and the left testis was just deep to the deep ring. There was clear evidence of a uterus cervix with bilateral fallopian tubes behind the urinary bladder [Figure 3]. On the operating table, cytology from both the testes was obtained, and no viable spermatozoa were detected on the right side, whereas motile sperms were visualized on the left side. The right orchiectomy was performed along with the removal of Müllerian remnants (hysterectomy with bilateral salpingectomy). Single-stage orchidopexy was done for the left testis [Figure 4]. The patient had an uneventful recovery and was discharged on 3rd post-operative day. Histopathology study of the left testis showed features of Sertoli cell-only syndrome, right testis, uterus, cervix, and bilateral fallopian tubes showed features of PMDS.

- Intraoperative image confirming presence of uterus and fallopian tubes in pelvis and intraabdominal right testis, left testis at inguinal region pulled into abdomen to confirm.
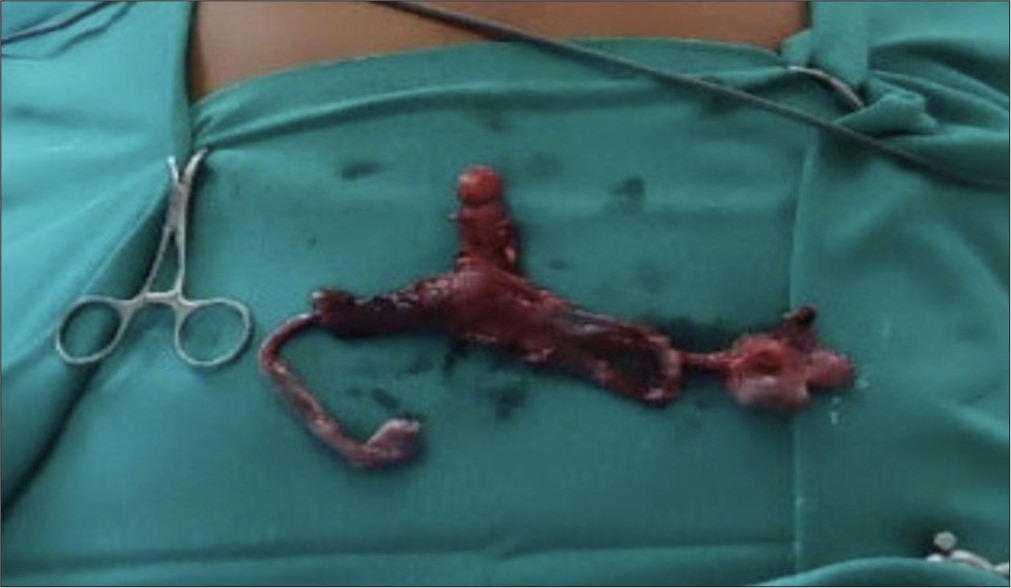
- Specimen of Hysterectomy with bilateral salpingectomy and right orchidectomy.
On subsequent follow-up, scrotal Doppler revealed normal testis on the left side scrotal sac with good blood flow. The semen analysis after 3 months of surgery showed improvements in semen parameters.
DISCUSSION
Up until the eighth week of pregnancy, the male fetus had Müllerian system derivatives; however, regression began as a result of a rise in MIS, which is generated by the testis’ Sertoli cells.[1,2] In a healthy individual, the prostatic utricles are the only remaining remnants of the Müllerian system.
PMDS, or the persistence of Müllerian structure, is caused by defects in the end organ activation of MIS, production failures, or release failures.[3,4] PMDS can be X-linked or an autosomal recessive sex-linked characteristic, or it can occur infrequently.[5] The Müllerian inhibiting substance receptor gene-II mutation is transmitted autosomally by recessive inheritance.[6,7] Approximately 85% of all cases have the mutation.
Although, PMDS is a congenital condition, patients can visit a doctor at any age, even before or after getting married. Due to their well-developed scrotum, patients may not be aware that they are missing their testicles until their spouse notices them or the surgeon examines them. In our instance, the patient’s reproductive problem led to their presentation at age 25.
Three types of PMDS exist: (1) Female type (60–70%) with bilateral intra-abdominal testes and epididymis connected to fallopian tubes in a position similar to ovaries; (2) hernia uteri inguinalis (20–30%) with a testis present in the scrotum and a contralateral testis present in the abdomen; and (3) transverse testicular ectopic (10%) with both testes present in the same hernia sac as the uterus and fallopian tubes.[4,8,9]
Classifying PMDS with a clinical examination is challenging when fallopian tubes and testicles should be further explored by a patient who has bilateral cryptorchidism. The presence of uterus in the patient explored using an MRI or USG scan. The care of bilateral intra-abdominal testis in PMDS is a rare entity that depends on the diagnosis, additional counseling, and the best surgical technique.[10]
Repositioning the testis and conducting a hysterectomy with bilateral salpingectomy are the two main surgical procedures used to treat PMDS with the goal of preserving fertility.[7,11] If the procedure was done after the age of 25, frozen biopsies might play a significant role.
The orchidectomy is indicated if intraoperative is suspicious of malignancy or in a situation where the testis cannot be mobilized. In our presented case, the age at presentation was 25 years, and the testis was in the right iliac fossa. Through intraoperative frozen section study we confirmed spermatozoa absent in the right testis. We proceeded for laparoscopic orchidectomy, hysterectomy, and bilateral salpingectomy with orchiopexy of the left testis.
Excision of the Müllerian derivative material is necessary to avoid the uterus’s enlargement during sexual maturation and the blood clot that causes discomfort and formation of lower abdominal mass.[3,7,8]
Laparoscopic management of PMDS with bilateral cryptorchidism is reported by El-Gohary.[5] The diagnostic laparoscopy can be performed to assess the internal gonadal status and subsequent management plan. Laparoscopy not only aids in the diagnosis but also allows for the excision of Müllerian duct remnants and orchidectomy/orchidopexy.[5,9]
CONCLUSION
PMDS is a rare male internal sexual disorder characterized by normal phenotype 46 XY male with female reproductive structure due to mutation in the gene encoding for AMH or its receptor. The condition is usually diagnosed incidentally/during surgery or for the evaluation of primary infertility. Fertility is rare but possible if at least one testis is scrotal and its excretory ducts are intact. Most of the patients had normal testicular histology, which might allow fertility. The early diagnosis of PMDS makes possible the excision of Müllerian structures and a primary orchidopexy. The Müllerian structures should be removed whenever possible to avoid the risk of malignant transformation. The MRI imaging and then the laparoscopic approach give excellent visualization magnification and documentation regarding the treatment decision.
Acknowledgment
The authors acknowledged the faculties of the Department of Radiology, Reproductive Medicine, and Pathology of Ganni Subhalakshmi Medical College and General Hospital, Rajahmundry, Andhra Pradesh.
Ethical approval
The research/study complied with the Helsinki Declaration of 1964.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship: Nil.
References
- Persistent Müllerian duct syndrome with bilateral abdominal testis: Surgical approach and review of the literature. J Pediatr Urol. 2005;1:423-7.
- [CrossRef] [PubMed] [Google Scholar]
- The delicate balance between male and female sex determining pathways: Potential for disruption of early steps in sexual development. Int J Androl. 2010;33:252-8.
- [CrossRef] [PubMed] [Google Scholar]
- Persistent Müllerian duct syndrome: Report of two boys with associated transverse testicular ectopia. J Pak Med Assoc. 1999;49:74-6.
- [Google Scholar]
- Persistent Müllerian duct syndrome: How to deal with the Müllerian duct remnants-A review. Indian J Surg. 2010;72:16-9.
- [CrossRef] [PubMed] [Google Scholar]
- Laparoscopic management of persistent Müllerian duct syndrome. Paediatr Surg Int. 2003;19:533-6.
- [CrossRef] [PubMed] [Google Scholar]
- AMH and AMH receptor defects in persistent Müllerian duct syndrome. Hum Reprod Update. 2005;11:351-6.
- [CrossRef] [PubMed] [Google Scholar]
- Persistent Müllerian duct syndrome (PMDS): A rare anomaly the general surgeon must know about. Indian J Surg. 2015;77:217-21.
- [CrossRef] [PubMed] [Google Scholar]
- Management of the patients with persistent Müllerian duct syndrome: Is the ultimate goal testicular descent? Turk J Urol. 2018;44:166-71.
- [CrossRef] [PubMed] [Google Scholar]
- A case of persistent Müllerian duct syndrome diagnosed by laparoscopic examination for impalpable testis. Hinyokika Kiyo. 2012;58:507-9.
- [Google Scholar]
- Laparoscopic management of persistent Müllerian duct syndrome. Indian J Surg. 2015;77:217-21.
- [Google Scholar]
- Persistent Müllerian duct syndrome. Indian J Pathol Microbiol. 2009;52:546-8.
- [CrossRef] [PubMed] [Google Scholar]







