Translate this page into:
Gynecological outcomes of uterine niche after cesarean section: A descriptive study

*Corresponding author: Eman Aly Abdelfattah Assisstant professor, Department of Obstetrics and Gynecology, Alexandria University, Alexandria, Egypt. eman0eman0eman7@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Abdelfattah E.A, Abd- El Dayem T.M, Galal H.M, Taylon S.S. Gynecological outcomes of uterine niche after cesarean section: A descriptive study. J Reprod Healthc Med 2021;2:5.
Abstract
Objectives:
Our aim was to study the prevalence of isthmocele in cases with previous cesarean section scar presented to El Shatby maternity university hospital and its association with gynecological complications.
Material and Methods:
After approval of the ethics committee of Alexandria faculty of medicine, a sample of 300 patients delivered by cesarean section since 6 months or more presented by one or more of the following symptoms: Abnormal uterine bleeding (AUB) dysmenorrhea, secondary infertility, and lower abdominal pain were selected from the gynecology clinic of El Shatby maternity university hospital. All patients were subjected to history taking, clinical, and gynecological examination. Post-menstrual 2D transvaginal ultrasonography was done. Where the niche or isthmocele was seen as triangular or dome- shaped echo-free space. Data were collected and entered to the computer using Statistical Package for the Social Science program for statistical analysis.
Results:
Niche was found in 44 cases. Most of them were symptomatic. Duration from the last (CS) was statistically significant. Symptoms were related to number of previous cesarean sections.
Conclusion:
The incidence of post-cesarean section niche in El Shatby Maternity hospital was 14.67%. Most common symptoms were AUB and dyspareunia.
Keywords
Cesarean section
Niche
Gynecological symptoms
INTRODUCTION
Cesarean delivery is the most common major surgery performed in the world, and its rate is rapidly increasing.[1]
A relatively new long-term sequela is the niche also called uterine scar dehiscence, cesarean scar defects, isthmocele and pouch. It is defined as “an indentation at the site of the uterine caesarean scar with a depth of at least 2 mm on ultrasound.”[2] It is present in 56–84% of women after one or more cesarean sections.[3] It is associated with multiple symptoms: abnormal uterine bleeding (AUB), for example, prolonged menstruation and post-menstrual spotting, which is present in 30% of women with a niche.[3] Other symptoms include dysmenorrhea and chronic pelvic pain.[4] Furthermore, the retention of blood, mucus, and fluid in the niche, cervix, and uterus is hypothesized to be a cause of secondary subfertility, due to unsuccessful sperm cell penetration or embryo implantation.[5]
The relationship between various niche features and symptoms has not been fully elucidated, although both niche volume and the “healing ratio” (residual myometrial thickness/adjacent myometrial thickness) have been reported to be associated with AUB.[6,7]
A niche can cause obstetric complications as well, such as niche pregnancies, mal-placentation, and uterine rupture.[8-10]
In this study, we aim at studying the prevalence of isthmocele in cases with previous cesarean section scar presented to El Shatby Maternity University Hospital and its association with gynecological complications.
MATERIAL AND METHODS
After approval of the Ethics Committee of Alexandria Faculty of Medicine, a sample of 300 patients delivered by cesarean section since 6 months or more (the last day cutoff was 15th of May 2019) was selected from the gynecology clinic of El Shatby maternity university hospital. They were presented by one or more of the following symptoms: AUB, dysmenorrhea, secondary infertility, or lower abdominal pain. Prior myomectomy or any pelvic pathology as uterine or ovarian swellings, or endometriosis was excluded from the study.
All patients were subjected to history taking, clinical, and gynecological examination. Post-menstrual 2D transvaginal ultrasonography was done. Cases were examined in the lithotomy position by a high quality machine (Voluson P8 General electric) where the niche or isthmocele was seen as triangular or dome-shaped echo-free space.[11,12]
Statement of ethics
The procedures followed were assessed by the responsible review committee (ethics committee of Alexandria Faculty of Medicine) and informed consent of patients was obtained.
Statistical methodology
Data were collected and entered into the computer using Statistical Package for the Social Science program for statistical analysis (ver 21).[13] Data were entered as numerical or categorical, as appropriate.
Kolmogorov–Smirnov test of normality revealed significance in the distribution of some variables, so the non-parametric statistics was adopted.[14]
Data were described using minimum, maximum, mean, standard deviation, and 95% CI of the mean[15] and also using median and inter-quartile range for not-normally distributed data
Categorical variables were described using frequency, percentage, and 95% CI of proportion (percentage)[16,17]
Histogram with normal curve, Box and Whiskers, and bar chart graphs were used accordingly.
An alpha level was set to 5% with a significance level of 95% (except for multiple comparisons), and a beta error accepted up to 20% with a power of study of 80%.
RESULTS
This study was carried on 300 patients with previous cesarean section scar. The age ranged from 18 to 40 years with a mean of 29.32 ± 5.862 years (95% CI for mean 28.65–29.98 years). Statistically, age was not normally distributed (D = 0.079, P = 0.000) so a median (IQR) of 29.00 (25.00–33.50) years was used in description [Figure 1].
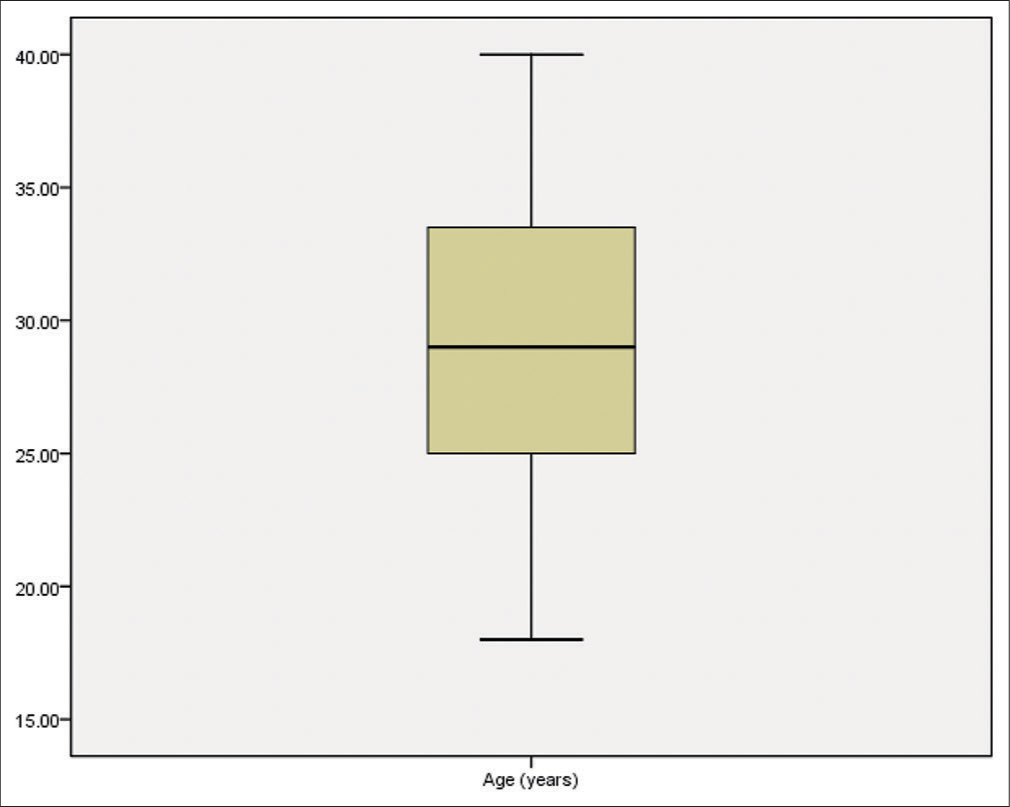
- Box and whisker graph of age (years) in the studied group, the thick line in the middle of the box represents the median, the box represents the inter-quartile range (from 25th to 75th percentiles), the whiskers represents the minimum and maximum.
One hundred seventy-six (58.67%) patients had a gravidity of 1 to 2, 116 (38.67%) patients had a gravidity of 3–4, and 8 (2.67%) patients had a gravidity of 5 or more [Figure 2].
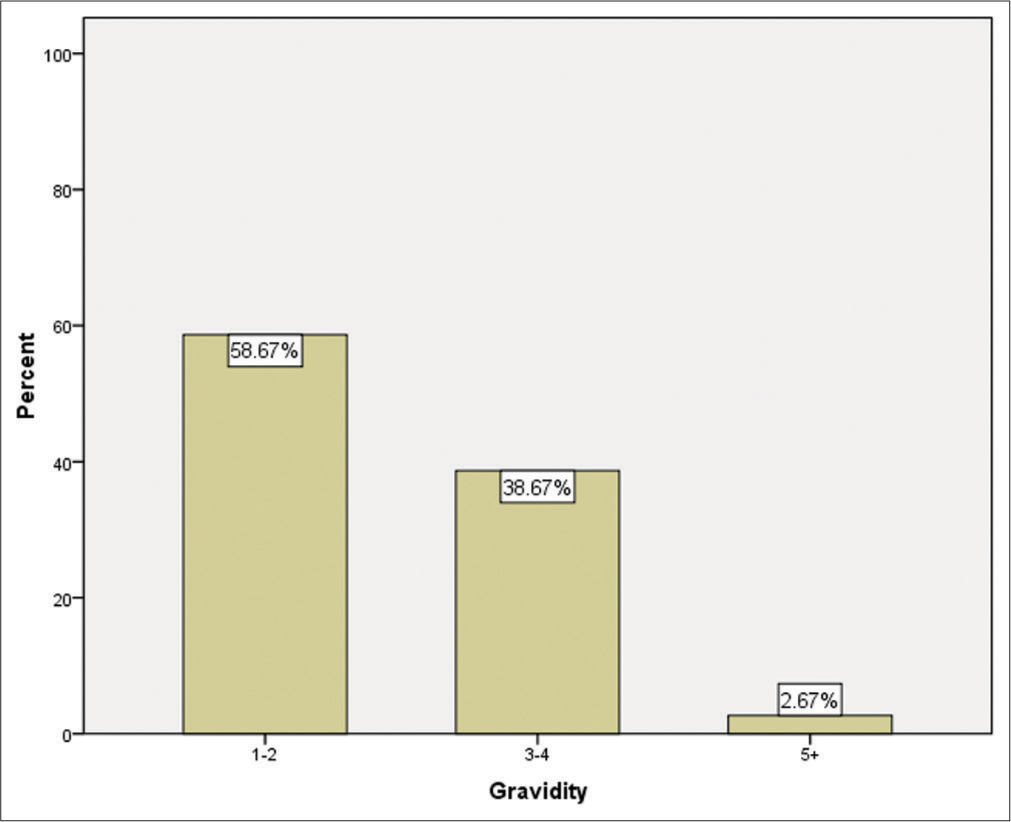
- Bar chart showing gravidity in the studied group.
As regards parity, 194 (64.67%) patients had a parity of 1–2, 102 (34.00%) patients had a parity of 3–4, and 4 (1.33%) patients had a parity of 5 or more [Figure 3].
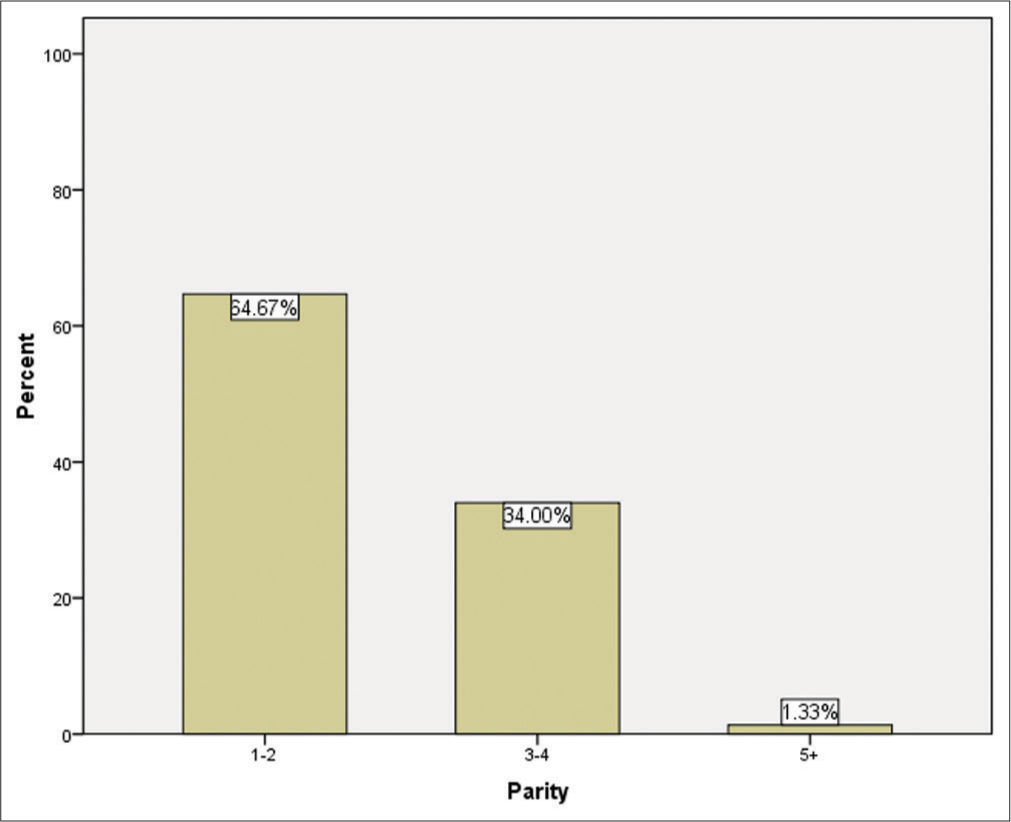
- Bar chart showing parity in the studied group.
One hundred fifteen (38.33%) patients had only 1 previous CS, 116 (38.67%) patients had 2 previous CS, 67 (23.33%) had 3 previous CS, and 2 (0.67%) had 4 previous CS [Figure 4].
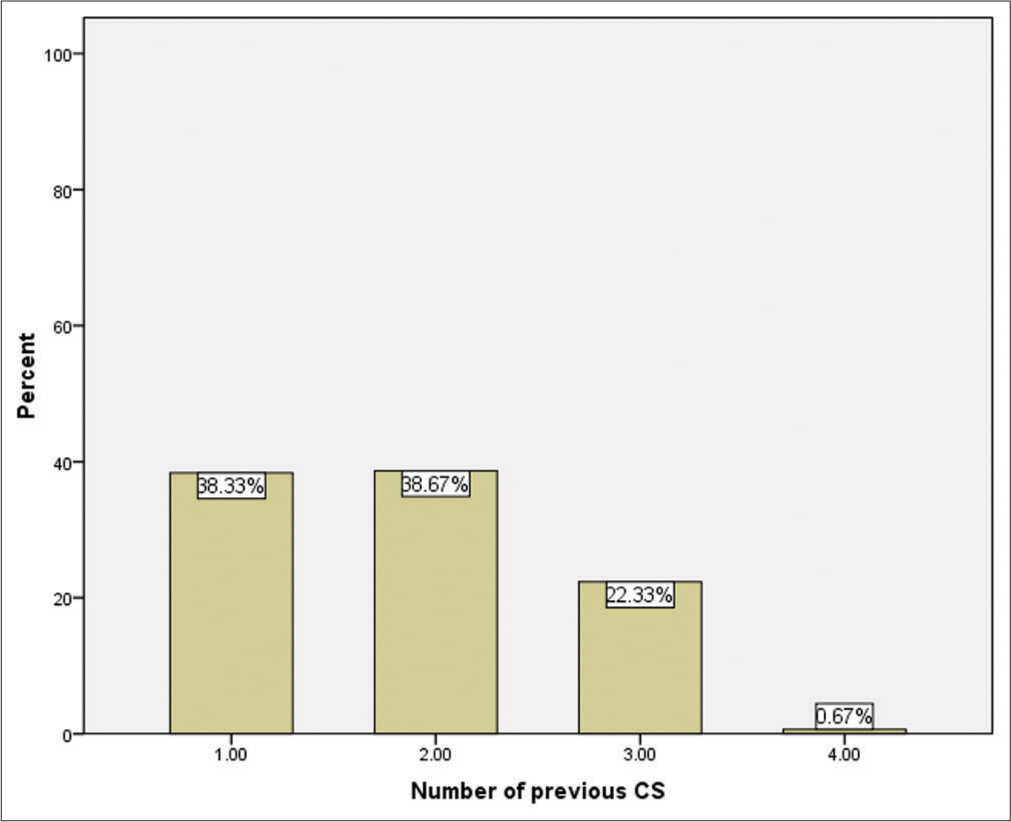
- Bar chart showing number of previous CS in the studied group.
The previous mode of delivery within the whole sample was studied; 43 (14.33%) of patients had previous NVD, 15 patients (34.88%) had NVD once, 19 patients (44.19%) had NVD twice, and 9 patients (20.93%) had NVD 3 times. Thirty-eight patients (12.6%) had previous CS; 26 of them (68.42%) had CS once, and 12 (31.58%) had CS twice. Thirty-one patients (10.33%) had abortion; 20 (64.52%) of them had 1 abortion, 7 (22.58%) had 2 abortions, and 4 (12.90%) had 3 or more abortions.
Participants were studied as regards parity, history of previous CS, position of the uterus, and thinned scar. Only history of previous CS and position of the uterus were found statistically significant (previous CS; P= 0.044*, RVF;P= 0.001*, AVF;P= 0.002*) [Table 1].
| Niche | Test of significance | ||
|---|---|---|---|
| No (n=256) (%) | Yes (n=44) (%) | ||
| Parity | |||
| 1–2 | 170 (87.63) | 24 (12.37) | X2=3.494 |
| 3–4 | 82 (80.39) | 20 (19.61) | P(MC)=0.204 |
| 5+ | 4 (100.0) | 0 (0.0) | NS |
| Previous CS | |||
| 1 | 102 (88.70) | 13 (11.30) | X2=8.144 |
| 2 | 102 (87.9) | 14 (12.07) | P=0.044* |
| 3 | 50 (74.63) | 17 (25.37) | |
| 4 | 2 (100.0) | 0 (0.0) | |
| RVF uterus | |||
| No | 208 (88.9) | 26 (11.1) | X2=10.744 |
| Yes | 48 (72.73) | 18 (27.27) | P=0.001* |
| AVF uterus | |||
| No | 50 (73.53) | 18 (26.47) | X2=9.789 |
| Yes | 206 (88.79) | 26 (11.2) | P=0.002* |
| Thinned scar | |||
| No | 229 (84.19) | 43 (15.81) | X2(Y)=2.139 |
| Yes | 27 (96.43) | 1 (3.57) | P(Y)=0.144 NS |
Percentage calculated from row total. MC: Monte Carlo correction for P-value of Pearson Chi-square test. Y: Continuity (Yate’s) correction of Pearson Chi-square test. NS: Statistically not significant (P>0.05). *Statistically significant (P<0.05)
The duration since last CS time ranged from 0.5 to 10 years with a mean of 2.96 ± 2.302 years (95% CI for mean 2.96-2.302 years). Statistically the duration since last CS was not normally distributed (D = 0.150, P= 0.000) so a median (IQR) of 2.5 (1.00–4.00) years was better to be used in description. Out of the 300 included patients, 128 (42.32%) had emergency CS and 172 (57.33%) had elective CS [Figure 5].
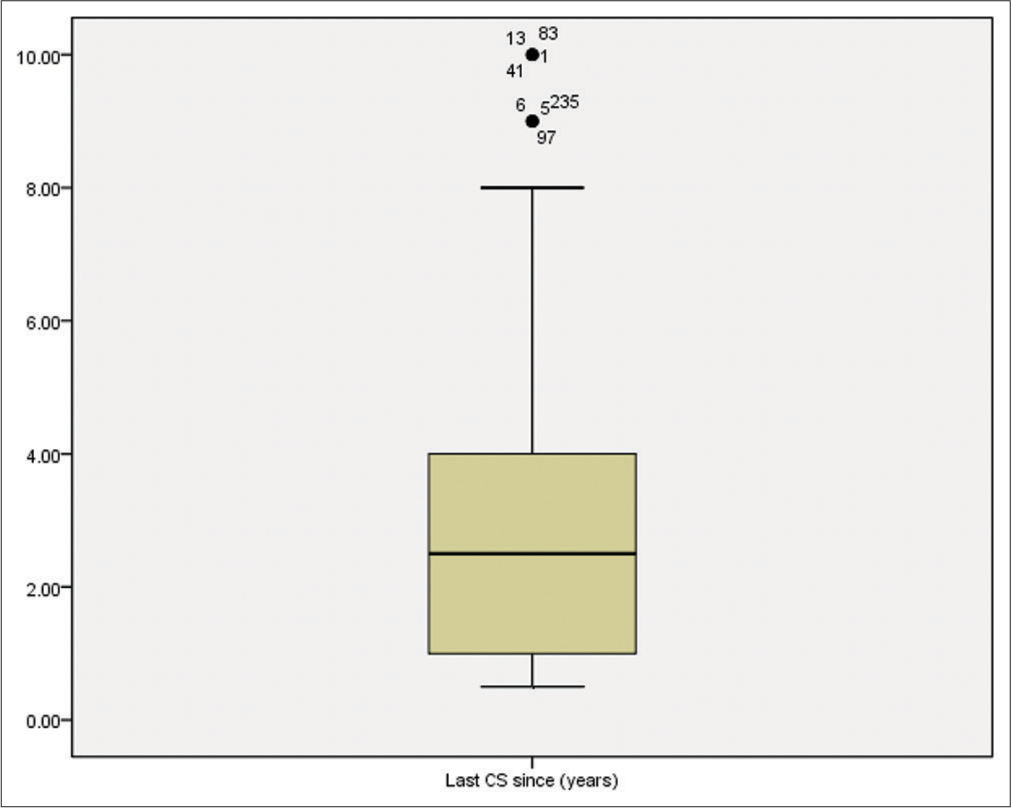
- Box and whisker graph of time since last CS since (years) in the studied group, the thick line in the middle of the box represents the median, the box represents the inter-quartile range (from 25th to 75th percentiles), the whiskers represents the minimum and maximum after excluding outliers (black-filled circle). Numbers indicate the serial number of the case in the master table.
In the present study, 76 (25.33%) patients had no complaints, they were presented by gynecological infections or pain due to complicated ovarian cyst and the niche was accidentally found while doing routine ultrasonography. One hundred and twenty-three patients (41.00%) complained of unexplained pelvic pain, 72 patients (24.00%) complained of AUB, 31 patients (10.33%) complained of secondary infertility, 4 patients (1.33%) complained of habitual abortion, 4 patients (1.33%) complained dyspareunia, 2 patients (0.67%) complained of stress incontinence, 2 patients (0.67%) complained of oligo-menstruation, and 2 patients (0.67%) complained of missed IUD [Figure 6].
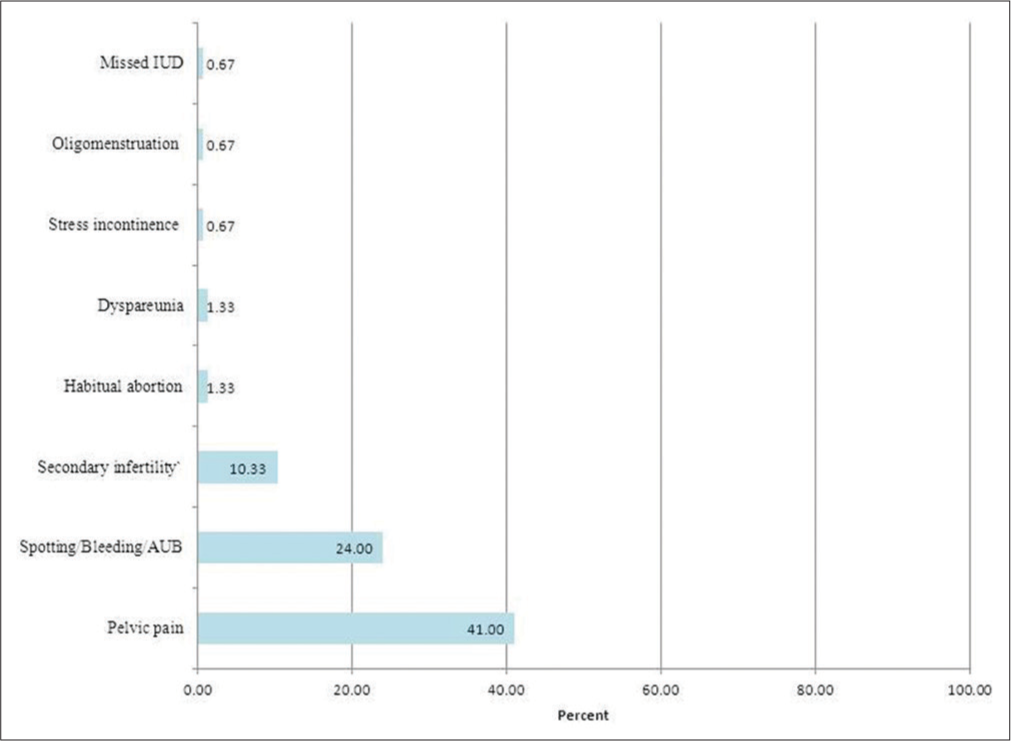
- Prevalence of different symptoms in the studied group.
In patients with niche (n = 44, 14.67%); 2 (4.55%) had no complaints, 15 (34.09%) complained of pelvic pain, 14 (31.82%) patients complained of secondary infertility, 13 (29.55%) patients complained of DUB, 4 (9.09%) patients complained of dyspareunia, and 2 (4.55%) patients complained of oligo-menstruation.
Patients with niche who had complaints were 42 cases (95.45%) which is more than the number with no niche and having complaints (n = 182) (71.09%) (P = 0.001). Thirteen patients (29.55%) with niche complained of DUB compared to 18 patients (7.03%) with no niche. This difference was statistically significant (P = 0.000).
Four patients had dyspareunia all of them (100%) had niche. Compared with patients with no niche, a statistical significant difference was found (P = 0.000).
Two patients had oligo-menstruation, all of them (100%) had niche, with statistical significant difference when compared with patients with no niche (p=0.016).
Four patients had habitual abortion, all of them (100%) had no niche. Compared with patients with niche no statistically significant difference was found (P = 0.902).
Two patients had stress incontinence, both (100%) had no niche but this was not statistically significant when compared to patients with niche (P = 1.000) [Table 2].
| Complaints | Patients with no niche (n=256) | Patients with niche (n=44) | Test of significance (P-value) |
|---|---|---|---|
| No complaints | |||
| n | 74 | 2 | X2(df=1)=11.780 |
| % Within symptom | 97.37% | 2.63% | P=0.001* |
| % Within niche | 28.91% | 4.55% | |
| Pelvic pain | |||
| n | 108 | 15 | X2(df=1)=1.018 |
| % Within symptom | 87.80% | 12.20% | P=0.313 NS |
| % Within niche | 42.19% | 34.09% | |
| Secondary infertility | |||
| n | 58 | 14 | X2(df=1)=1.728 |
| % Within symptom | 80.56% | 19.44% | P=0.189 NS |
| % Within niche | 22.66% | 31.82% | |
| AUB | |||
| n | 18 | 13 | X2(Y)(df=1)=18.183 |
| % Within symptom | 58.06% | 41.94% | P(Y)=0.000* |
| % Within niche | 7.03% | 29.55% | |
| Habitual abortion | |||
| n | 4 | 0 | X2(Y)(df=1)=0.015 |
| % Within symptom | 100.00% | 0.00% | P(Y)=0.902 NS |
| % Within niche | 1.56% | 0.00% | |
| Dyspareunia | |||
| n | 0 | 4 | X2(Y)(df=1)=17.183 |
| % Within symptom | 0.00% | 100.00% | P(Y)=0.000* |
| % Within niche | 0.00% | 9.09% | |
| Stress incontinence | |||
| n | 2 | 0 | X2(Y)(df=1)=0.000 |
| % Within symptom | 100.00% | 0.00% | P(Y)=1.000 NS |
| % Within niche | 0.78% | 0.00% | |
| Oligo-menstruation | |||
| n | 0 | 2 | X2(Y)(df=1)=5.856 |
| % Within symptom | 0.00% | 100.00% | P(Y)=0.016* |
| % Within niche | 0.00% | 4.55% | |
| Missed IUD | |||
| N | 2 | 0 | X2(Y)(df=1)=0.000 |
| % Within symptom | 100.00% | 0.00% | P(Y)=1.000 NS |
| % niche | 0.78% | 0.00% |
X2: Pearson Chi-square test. df: Degree of freedom. Y: Yate’s (continuity correction) for Pearson Chi-square test and its P-value. NS: Statistically not significant (P>0.05). *Statistically significant (P<0.05)
As regards description of the CS scar by TVUS; 230 (76.67%) of patients had good capitation, 44 (14.67%) had niche, 28 (9.33%) had thinned scar, and 5 (1.67%) had scar straight [Table 3 and Figure 7].
| Description of the CS scar by TVUS | n(n=300) | % (Within total) (95% CI) |
|---|---|---|
| Good capitation | 230 | 76.67 (71.39–81.25) |
| Niche | 44 | 14.67 (10.97–19.30) |
| Thinned scar | 28 | 9.33 (6.39–13.34) |
| Scar straight | 5 | 1.67 (0.62–4.07) |
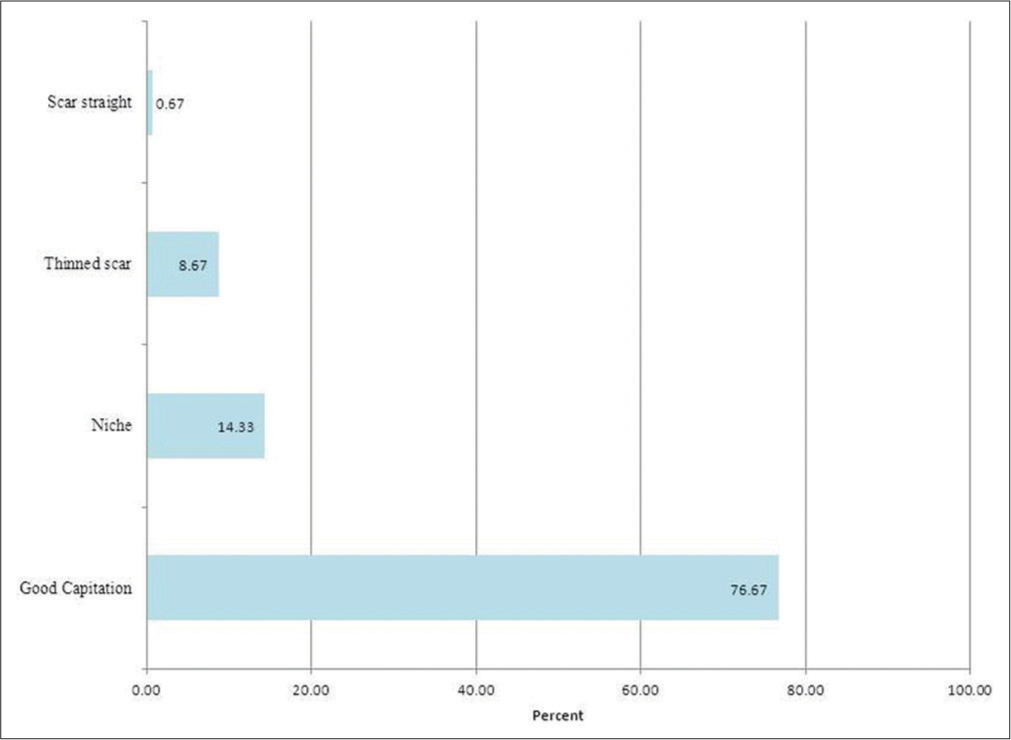
- Prevalence of different CS scar description by TVUS.
In patients who had niche, only 1 (2.27%) had good capitation, 1 (2.27%) had thinned scar, and 1 (2.27%) had scar straight [Table 4].
| Description of the CS scar by TVUS | n(n=44) | % (within total) (95% CI) |
|---|---|---|
| Good capitation | 1 | 2.27 (0.12–13.51) |
| Thinned scar | 1 | 2.27 (0.12–13.51) |
| Scar straight | 1 | 2.27 (0.12–13.51) |
The uterus was AVF in 232 (77.33%) patients, RVF in 66 (22.00%) patients, and unicornuate in 2 (0.67%) patients. When comparing both groups as regards; parity, previous CS, position of the uterus and thinned scar, no statistically significant difference was found except for position of the uterus (RVF: P= 0.001*, AVF: P= 0.002*).
DISCUSSION
The reported number of cesarean sections in Egypt is high. Increasing number of this procedure is inseparably connected with the rising number of intra- and post-surgical complications.[18] Uterine scar dehiscence after cesarean section is described in literature as “isthmocoele,” “niche,” “pouch,” or “cesarean scar defect.”[19]
Two studies reported that closure technique during CS affects niche development assuming that double-layer or full thickness suturing is more appropriate.[20] In our center, we use double layer closure more than single layer closure yet we have high prevalence of uterine niche which could be due to other etiologies such as continuous suturing, sometimes anchored on the myometrium which is more ischemic compared to suturing by separate stitches. Correlating the type of uterine suturing and presence of isthmocele is important to avoid effect of this post-operative complication on the quality of life (QoL) of women for years.[20]
In our sample, 44 (14.67%) patients had niche of the CS scar by TVUS. This finding is much less than that reported by de Vaate et al. (2014), in their systematic review, where they found the prevalence CS niche ranged from 56% to 84% when using contrast-enhanced sonohysterography in a random population of women with a history of CS.[21]
de Vaate et al. (2014)[21] hypothesized that potential factors affecting the development of the lower uterine segment (such as duration of labor, dilatation, and stage of the presenting part) may also influence the development of a niche.
Characteristics of the myometrium alter during labor, a thinner myometrium may be less well vascularized, which may lead to insufficient wound healing and niche development.[22] In addition, a lower position of the CS incision, especially in the cervical part of the uterus, may be more prone to the development of a niche.[23]
Fortunately, in most cases the niche is asymptomatic but sometimes it may cause symptoms which may decrease QoL.[18] Since nearly one in three women undergoes cesarean delivery, a comprehensive understanding of a woman’s experience and subsequent QoL after surgery is important.[24]
AUB is a common complaint among women of reproductive age, most of the times stemming from functional disorders of the menstrual cycle or as a result of uterine diseases, such as polyps, myomas, and endometrial hyperplasia.[25,26] Bleeding could be intermenstrual or post-menstrual spoting.
The predominant symptom related to a niche is post-menstrual spotting. Borges et al. (2010)[27] reported that 88% of patients submitted to hysteroscopy had a diagnosis of isthmocele matching with literature.
Nonetheless, the anatomic defect on the anterior uterine wall, caused by a prior cesarean section, must be considered in the differential diagnosis. Only one study performed in a random population described a positive relationship between a niche and post-menstrual spotting.[28] This association was not found by Valenzano et al.,[29] who denied the relationship between post-menstrual spotting and a previous CS.
This discrepancy in the findings of these two studies can be explained by variations in methodology such as definition of a niche, timing of the ultrasound scans, and exclusion of multiple CSs in the population of Valenzano et al.[29]
According to Monteagudo et al.,[11] the presence of a niche on transvaginal ultrasonography was also related to intermenstrual bleeding. Such defect was found in 82.6% of women with intermenstrual bleeding and past history of cesarean section.
In 1995, Morris[30] analyzed 51 uterine samples of women who underwent hysterectomy for AUB not responsive to medical treatment without identifiable uterine abnormalities. These women previously underwent cesarean section. Morris[30] found that the scar tissue contributed to a series of pathologic changes, including distortion and widening of the lower uterine segment (75%), “overhang” of congested endometrium above the scar recess (61%), polyp formation conforming to the contours of the scar recess (16%), moderate to marked lymphocytic infiltration (65%), residual suture material with foreign body giant cell reaction (92%), capillary dilatation (65%), free red blood cells in the endometrial stroma of the scar suggesting recent hemorrhage (59%), fragmentation and breakdown of the endometrium of the scar (37%), and iatrogenic adenomyosis confined to the scar (28%).
The etiopathogenesis of the “isthmocele” is unknown. The uterine incision generally is made transversely in the lower segment anatomically decreasing the risk of dehiscence in future pregnancies. However, the superior edge of the incision is thicker than the inferior edge, and this discrepancy increases with the increase in the number of cesarean deliveries.[31] Thurmond et al.[31] suggested the development of a reservoir-like “pouch,” where residual menstrual blood accumulates. Furthermore, Thurmond et al.[31] suspected that this condition depends not only on the size or location of the scar but also on poor contractility of the uterine muscle around the scar, which could obstruct menstrual blood drainage, causing its accumulation in the defect. Nevertheless, it cannot be excluded that the accumulated blood may be produced in situ, as suggested by Morris[30] based on the presence of free red blood cells in the endometrial stroma, suggesting recent hemorrhage.
The presence of fibrotic tissue in the niche acts like a valve, leading to the accumulation of blood in this reservoir-like area thus causing delayed menstruation through the cervix, resulting in abnormal bleeding, pelvic pain, vaginal discharge, dysmenorrhea, dyspareunia, and infertility. Accumulated blood can ultimately degrade cervical mucus and sperm quality and it can also inhibit sperm transport presenting a proposed mechanism of infertility.[25] Women with a niche who conceive are at potential risk for cesarean scar ectopic pregnancy, with the embryo implanting in the pouch.
In the majority of the studies evaluating niches in women with gynecological symptoms, selection bias is likely to play a role.[20,32]
The higher prevalence of persisting dyspareunia in women who had an operative birth raises important questions about the longer-term impact of operative procedures on women’s health. Few prospective studies have collected data on the persistence of dyspareunia beyond 6 months postpartum.
Almost all women experience some pain during sexual intercourse following childbirth. Some studies found that the odds of dyspareunia at 18 months were substantially higher in women who delivered by vacuum extraction or vaginal birth assisted with forceps compared with women who had a spontaneous vaginal birth with an intact perineum and somewhat higher for women who had an elective cesarean section rather than an emergency cesarean section. Alternatively, it is possible that women recover more quickly from forceps than from vacuum extraction and that women having an elective cesarean section that does experience postpartum dyspareunia are slow to recover.[33]
In our study, dyspareunia was statistically significant in the niche group although other factors may be associated including pre-pregnancy dyspareunia, intimate partner abuse, and maternal fatigue.
Strengths and limitations
We used a 2-D ultrasound but using a 3-D ultrasound should have been more useful. Similarly, MRI is a better modality for niche diagnosis. They would have picked up more cases or would have been better but could not be done due to financial constraints.
CONCLUSION
The incidence of post-cesarean section niche in El Shatby Maternity hospital was 14.67% which increases with the increased number of cesarean section. Most common complaints were AUB and dyspareunia. Symptoms are more common among emergency cesarean section than elective cesarean section.
Acknowledgments
Special thanks to doctor El-Sayed Amr for his co-operation in statistics, and to nursing staff of El-Shatby Hospital for their co-operation.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- The increasing trend in caesarean section rates: Global, regional and national estimates: 1990-2014. PLoS One. 2016;11:e0148343.
- [CrossRef] [PubMed] [Google Scholar]
- Sonographic examination of uterine niche in non-pregnant women: A modified Delphi procedure. Ultrasound Obstet Gynecol. 2019;53:107-15.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence, potential risk factors for development and symptoms related to the presence of uterine niches following Cesarean section: Systematic review. Ultrasound Obstet Gynecol. 2014;43:372-82.
- [CrossRef] [PubMed] [Google Scholar]
- Cesarean scar defect: Correlation between cesarean section number, defect size, clinical symptoms and uterine position. Ultrasound Obstet Gynecol. 2009;34:85-9.
- [CrossRef] [PubMed] [Google Scholar]
- Why do niches develop in Caesarean uterine scars? Hypotheses on the aetiology of niche development. Hum Reprod. 2015;30:2695-702.
- [CrossRef] [PubMed] [Google Scholar]
- Ultrasound evaluation of the Cesarean scar: Relation between a niche and postmenstrual spotting. Ultrasound Obstet Gynecol. 2011;37:93-9.
- [CrossRef] [PubMed] [Google Scholar]
- Long-term complications of caesarean section. The niche in the scar: A prospective cohort study on niche prevalence and its relation to abnormal uterine bleeding. BJOG. 2014;121:236-44.
- [CrossRef] [PubMed] [Google Scholar]
- Cesarean scar pregnancy and placenta accreta. Ultrasound Obstet Gynecol. 2014;43:361-2.
- [CrossRef] [PubMed] [Google Scholar]
- Therapeutic options of caesarean scar pregnancy: Case series and literature review. J Clin Ultrasound. 2010;38:75-84.
- [CrossRef] [PubMed] [Google Scholar]
- Prediction of complete uterine rupture by sonographic evaluation of the lower uterine segment. Am J Obstet Gynecol. 2009;201:320.e1-6.
- [CrossRef] [PubMed] [Google Scholar]
- Saline infusion sonohysterography in nonpregnant women with previous cesarean delivery: The niche in the scar. J Ultrasound Med. 2001;20:1105-15.
- [CrossRef] [PubMed] [Google Scholar]
- Resectoscopic correction of the “isthmocele” in women with postmenstrual abnormal uterine bleeding and secondary infertility. J Minim Invasive Gynecol. 2008;15:172-5.
- [CrossRef] [PubMed] [Google Scholar]
- Discovering Statistics Using IBM SPSS Statistics (4th ed). London, California, New Delhi: SAGE Publications Ltd; 2013.
- [Google Scholar]
- Two-sided confidence intervals for the single proportion: Comparison of seven methods. Stat Med. 1998;17:857-72.
- [CrossRef] [Google Scholar]
- Probable inference, the law of succession, and statistical inference. J Am Stat Assoc. 1927;22:209-12.
- [CrossRef] [Google Scholar]
- When and how should we treat cesarean scar defect-isthmocoele? Ginekol Pol. 2016;87:664-8.
- [CrossRef] [PubMed] [Google Scholar]
- The cesarean delivery scar pouch: Clinical implications and diagnostic correlation between sonography and hysteroscopy. J Ultrasound Med. 2003;22:695-700.
- [CrossRef] [PubMed] [Google Scholar]
- Methods for myometrium closure and other factors impacting effects on cesarean section scars of the uterine segment detected by the ultrasonography. Acta Obstet Gynecol Scand. 2017;85:429-34.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence, potential risk factors for development and symptoms related to the presence of uterine niches following Cesarean section: Systematic review. Ultrasound Obstet Gynecol. 2014;43:372-82.
- [CrossRef] [PubMed] [Google Scholar]
- The effect of dystocia and previous cesarean uterine scar on the tensile properties of the lower uterine segment. Am J Obstet Gynecol. 2006;194:873-83.
- [CrossRef] [PubMed] [Google Scholar]
- High prevalence of defects in Cesarean section scars at transvaginal ultrasound examination. Ultrasound Obstet Gynecol. 2009;34:90-7.
- [CrossRef] [PubMed] [Google Scholar]
- Caesarean section: Could different transverse abdominal incision techniques influence postpartum pain and subsequent quality of life? A systematic review. PLoS One. 2015;10:e0114190.
- [CrossRef] [PubMed] [Google Scholar]
- Surgical treatment and follow-up of women with intermenstrual bleeding due to cesarean section scar defect. J Minim Invasive Gynecol. 2005;12:25-8.
- [CrossRef] [PubMed] [Google Scholar]
- Ultrasonographic evaluation of lower uterine segment to predict the integrity and quality of cesarean scar during pregnancy: A prospective study. Tohoku J Exp Med. 1997;183:55-65.
- [CrossRef] [PubMed] [Google Scholar]
- Findings in patients with postmenstrual spotting with prior cesarean section. J Minim Invasive Gynecol. 2010;17:361-4.
- [CrossRef] [PubMed] [Google Scholar]
- Ultrasound evaluation of the Cesarean scar: Relation between a niche and postmenstrual spotting. Ultrasound Obstet Gynecol. 2011;37:93-9.
- [CrossRef] [PubMed] [Google Scholar]
- Vaginal ultrasonographic and hysterosonographic evaluation of the low transverse incision after caesarean section: Correlation with gynaecological symptoms. Gynecol Obstet Invest. 2006;61:216-22.
- [CrossRef] [PubMed] [Google Scholar]
- Surgical pathology of the lower uterine segment caesarean section scar: Is the scar a source of clinical symptoms? Int J Gynecol Pathol. 1995;14:16-20.
- [CrossRef] [PubMed] [Google Scholar]
- Cesarean section scar as a cause of abnormal vaginal bleeding: Diagnosis by sonohysterography. J Ultrasound Med. 1999;18:13-6.
- [CrossRef] [PubMed] [Google Scholar]
- Changes in maternal characteristics and obstetric practice and recent increases in primary cesarean delivery. Obstet Gynecol. 2017;102:791-800.
- [CrossRef] [Google Scholar]
- Dyspareunia and childbirth: A prospective cohort study. BJOG. 2015;122:672-9.
- [CrossRef] [PubMed] [Google Scholar]






